At the Surrey Allergy Clinic we routinely use the Skin Prick Testing (SPT) method of allergy testing to diagnose common inhalant, environmental and food allergies.
By Dr. Adrian Morris
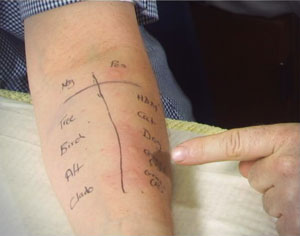 The skin of the inner forearm is the usual test site for allergy testing using the Skin Prick Test method. One can also take a blood sample for allergy testing and measure Total Immunoglobulin E (IgE) which is the marker antibody for allergy sensitisation. Then there are the Phadiatop inhalant screen, Food Allergy screens and over 450 individual RAST or ImmunoCAP tests available.
The skin of the inner forearm is the usual test site for allergy testing using the Skin Prick Test method. One can also take a blood sample for allergy testing and measure Total Immunoglobulin E (IgE) which is the marker antibody for allergy sensitisation. Then there are the Phadiatop inhalant screen, Food Allergy screens and over 450 individual RAST or ImmunoCAP tests available.
We can quantify allergy severity with another cellular marker, this is the Eosinophil cell in the blood stream. Eosinophils are also found in the allergy sufferer’s phlegm, gullet secretions and nasal mucous. Lung function tests are important in asthma diagnosis, and tests include Peak Flow (PF), Forced Expiratory Volume in 1 second (FEV1) and Forced Vital Capacity (FVC). Measurement of Nitric Oxide (NO) in exhaled air is another measure of allergic inflammation and indicates poor control or ineffective treatment.
Another method of determining if someone is allergic to a substance is to directly challenge him or her with that substance. This is called Challenge or Provocation allergy testing and is the Gold Standard in allergy diagnosis. But this is only practical in a controlled hospital environment as it can be dangerous and trigger a severe allergic reaction. Challenge tests include lung, conjunctiva and nasal challenges with the suspected allergen (for example pollen and mould spores) and Double Blind Placebo Controlled Food Challenge (DBPCFC) tests for suspected food allergy.
A positive allergy test indicates sensitisation to an allergen but does not necessarily predict that a clinically relevant allergic reaction will occur. That is why general allergy testing in otherwise healthy individuals is discouraged, as the results might be misleading. One should always question whether specific allergy symptoms can be linked to a particular allergy test result, and there can be no substitute for an expert allergist with years of experience in allergy testing, diagnosis and allergy treatment. The actual allergy consultation and process of “teasing out” details of the clinical allergy plus a full medical history in conjunction with specific allergy testing is pivotal to making an accurate allergy diagnosis.
Skin Prick or Scratch Allergy Testing
Skin Prick Testing (SPT) is one of the oldest allergy tests available and is the cornerstone of primary care allergy diagnosis. Allergy testing was first performed by Dr Charles Blackley who was a Manchester GP and Homeopath, to identify grass pollen as the cause for hay fever in 1865. This test is still the most highly sensitive allergy test available. It tests for specific Immunoglobulin E (IgE) antibodies to environmental allergens such as house dust mite, pollen, cat and dog dander but can also be used to test for food, insect venom and drug allergy. A positive result is a typically raised wheal and red flare reaction on the skin. It is used to either diagnose or exclude a specific IgE mediated cause for the patient’s allergic symptoms. Thus having good positive and negative predictive value in allergy diagnosis
The newer standardised glycerol based extracts (manufactured by ALK Abello, Inmunotek and Lofarma) are highly specific and accurate. They are cheap, safe and simple to perform if the tester has been trained to use them and the results are then immediately available. These tests are useful to demonstrate to the allergy sufferer, the acute inflammatory nature of allergy. They are particularly accurate in diagnosing the cause of asthma and rhinitis.
Prick and Prick tests are a variation of Skin Prick testing for food allergies and are performed using a drop of the fresh food extract. The skin is scratched pricked with a standard lancet through the drop of fresh food extract (for example fresh apple, melon or peach). This simple test is highly accurate when the correct lancet is used.
How are skin prick tests performed?
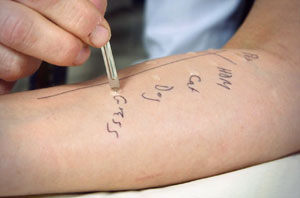 We use standardised glycerinated extracts of the various allergen extracts such as house dust mite, cat and dog dander, tree, grass and weed pollen and fungal spores. There is also a negative saline and positive histamine control (used as a quality control reference).
We use standardised glycerinated extracts of the various allergen extracts such as house dust mite, cat and dog dander, tree, grass and weed pollen and fungal spores. There is also a negative saline and positive histamine control (used as a quality control reference).
A droplet of each extract is placed on the inner aspect of the forearm about 3cm apart and we penetrate through the drop at 90 degrees to the skin using a specially modified lancet. Using firm controlled pressure and making sure not to draw blood.
The reactions are read after 15 to 20 minutes and a positive reaction should have at least 3mm of raised wheal. All oral antihistamine medication should be avoided for 2 – 3 days before hand, as these suppress skin reactivity.
Atopy Patch Tests
Atopy Patch Tests (APT) on the skin may detect delayed hypersensitivity reactions to foods, but are usually employed to identify trigger contact allergens such as nickel, rubber, dyes and cosmetics. However a new application of this patch test is to test for food allergens especially where a delayed (non-IgE) hypersensitivity reaction is suspected in children with Gastro Oesphageal Reflux (GOR), Eosinophilic Oesophagitis (EOE) disease and in delayed Atopic Eczema. The food allergen is applied to the skin under an occlusive cover (called a Finn chamber) and the skin is assessed after 48 and 72 hours for a wheal reaction. Any redness or micro-blistering is then measured and graded as a positive reaction.
Blood Testing for Allergy
 The original Total serum IgE blood test has been superseded by the newer multi-allergen screening tests. The inhalant allergy screen is called an ImmunoCAP Phadiatop and there are various ImmunoCAP food allergy screening panels such as the fx5 for common childhood food allergens, fx1 for nuts, fx2 for seafood’s and fx3 for cereals.
The original Total serum IgE blood test has been superseded by the newer multi-allergen screening tests. The inhalant allergy screen is called an ImmunoCAP Phadiatop and there are various ImmunoCAP food allergy screening panels such as the fx5 for common childhood food allergens, fx1 for nuts, fx2 for seafood’s and fx3 for cereals.
There are now over 450 individual ImmunoCAP or RAST tests available for everything from sheep dander to sesame seeds. A allergy screening test called ISAC can measure over 100 component allergens on a single blood sample and determines patterns of reactivity. The ALEX2 Component test has superseded the ISAC test with 240 individual allergen components measured in one screening test, available at many NHS and Private UK pathology reference laboratories.
Total serum IgE
Total Serum Immunoglobulin E or IgE was the original screening test for allergy, but has been superseded by newer more specific tests. However a Total IgE level exceeding 100kU/l is still highly suggestive of atopy or allergy in adults. Total IgE has a good predictive value in children under 3 years of age and may be used as a screening allergy test in this age-group. We used to measure Total Cord IgE on newborn babies umbilical cord blood at birth as a predictor of allergy, but this wasn’t accurate and is no longer recommended. The level of Total IgE depends on the number and size of organs affected by the allergy. For example, a skin allergy results in higher Total IgE than smaller organs such as allergy in the nose.
To confuse matters, Total IgE may also be raised in parasitic infections, some immune diseases, in cigarette smokers, with alcohol consumption and in certain cancers. Total IgE is not therefore 100% specific to allergy. Total IgE levels also depend on the size of the organ affected with allergies. It is relatively low in nose allergy, but very high in extensive skin allergy such as occurs with eczema. Levels naturally increase from infancy through to adolescence when they tend to plateau and then slowly decrease towards old age. There is a seasonal variation in Total IgE with levels peaking in spring for pollen allergic individuals.
The Phadiatop Inhalant allergy screen
The Phadiatop (which stands for Phadia Differential Atopy Test) is a multi-allergen inhalant allergy screening test – very useful for assessing if inhalant allergy is present in conditions such as asthma and rhinitis. It doesn’t tell us which individual allergens are implicated but rather whether there is respiratory allergy or not.
The screening panel has extracts of House dust Mite, Cat and Dog dander, Mould spores, Tree, Grass and Weed Pollen and can be adapted to include locally implicated aero-allergens such as Cockroach (a problem in North America).
Allergy Testing for childhood Food Allergy
The fx5 food allergy screen
The fx5 is the common Paediatric Food Allergy screening test that includes the commonest 6 implicated allergy-provoking foods. These are Cows Milk protein, Hens Egg white, Wheat, Codfish, Peanut and Soya bean. These foods account for 90% of IgE mediated food allergy in young children. The test is therefore a useful screening test in children when no individual food is obviously implicated or when multiple food allergies are suspected
fx1 Nut Allergy Screen
In older children and adults, nut allergy and anaphylaxis is an ever-increasing problem. The fx1 is a very useful screen for nut and peanut allergy and the screening panel includes Peanut, Hazelnut, Brazil nut, Almond and Coconut. It does not include Cashew, Pecan or Pistachio nut. In clinical practice, Peanut Cashew and Brazilnut account for most nut allergies but there is a considerable amount of cross-reactivity between the diverse botanical nut families.
In adults there is a seafood mix screen called fx2 which contains Codfish, Shrimp, Blue mussel, Tuna, and Salmon. The cereal grain mix screen called fx3 contains Wheat, Oat, Maize, Sesame seed and Buckwheat. Another useful food screen is the fx7, which mix contains Tomato, Yeast, Garlic, Onion and Celery. Screen tests tend to help reduce costs of allergy testing by selecting suspected food groups.
There are up to 160 different food allergens that can be used to test using the ImmunoCAP system for specific IgE food antibodies, and range from Almond through to Youngberry.
New technologies in Allergy Testing
Recombinant allergen components
Some foods such as cow’s milk and many fruits and nuts contain a large number of different potential allergens and one has to be aware that a specific RAST test may only test a few of the potential allergens in the food. Some people who are perhaps sensitised to a minor allergen in a particular food may RAST test negative, while in fact they are still highly allergic to that food.
For this reason an new range of recombinant allergens have been developed to measure specific proteins in food allergy. These individual proteins also called Profilin, PR-10 proteins, Tropomyosins and Lipid Transfer Proteins (LTPs) can occur in diverse unrelated foods such as Birch Pollen and Apple flesh or Latex and Avocado. As a result the unsuspecting Latex Allergy sufferer may have an acute allergic or anaphylactic reaction to Avocado, Banana, Kiwi or Chestnut when they eat these for the first time.
If the specific allergen is then identified on a blood test, the person can be advised exactly what foods they may react to and what foods to avoid. These recombinant allergen tests are however very expensive and one needs to do a vast number of specific tests to identify the major allergens.
For example in Hens’ egg, there are 4 different allergenic component proteins, called Gal d1 (Ovomucoid), Gal d 2 (Ovalbumin), Gal d 3 (Conalbumin) and Gal d 4 (Lysozyme). One or all of which could be the potential cause of an egg allergic reaction.
Cow’s Milk allergenic component proteins which may trigger allergic reactions include Bos d 4 (alpha-lactalbumin), Bos d 5 (beta-lactglobulin), Bos d 6 (Bovine serum albumin), Bos d 8 (Casein) and Bos d lactoferrin (Bovine lactoferrin)
Silver Birch pollen derived allergenic components include 5 different Bet v proteins including Profilin and LTP which cross react to various stone-fruits and nuts. Silver Birch allergic hay fever sufferers are particularly prone to oral allergic symptoms when eating fresh fruit and vegetables. This is called the Oral Allergy Syndrome (or Food Pollen Syndrome).
In Peanut we find 9 different Ara h allergens and in Latex 13 different Hev b allergens any of which could be the specific cause of Latex allergy.
The ImmunoCAP ISAC test (Thermo/PhaDia of USA) on a patients’ blood sample comprises 112 individual tests for component allergens, representing 52 different natural allergens. It is useful for patients with peanut allergy and latex allergy where identification of the individual components has clear implications for the treatment and the prognosis.
The new ALEX test (Macro-Array Diagnostics, of Vienna, Austria) comprises 126 component allergens plus 156 native allergens. That is therefore 262 tests in total, covering 167 different natural allergens. This much greater allergen panel is therefore not only useful for researching individual allergens for individual patients but is also a comprehensive and definitive allergen screening test for suspected allergic patients.
After a decade of use, the ISAC test is available within the NHS and from private laboratories for private practice Allergy Consultants. The very recently introduced ALEX test is so far available from a commercial service but will become available on the NHS soon.
These component IgE antibody screening tests are very useful in people who suffer with multiple food and inhalant allergies and helps identify to which group or groups of allergen they are cross-reacting such as profilins, LTPs, Tropomycins or CCDs. Once their cross-reactive allergen groups are identified, one can predict severity of future reactions and whether they would benefit from desensitization immunotherapy.
This can all be very confusing even to the experienced allergist! And this is why it is easier and cheaper allergy test using fresh food extracts for Skin Prick Testing to food allergies.
In summary, environmental, inhalant and food allergen identification using accurate allergy testing can be cost-effectively undertaken by the allergy practitioner utilising the following allergy tests with a well established record of reliability and reproducibility
Skin Prick Testing is the cornerstone in allergy diagnosis; it has been used for over 100 years. Skin testing is cheap, safe, and easy to do and someone in a GP practice can easily be trained to perform it. Commercial inhalant allergens are readily available, but food allergens are a little more difficult to manufacture. The main problem with food allergens is the lack of stability of extracts. A few food allergens such as Peanut, Egg, Wheat, Soya, Tree nuts, Fish and Sesame are stable and commercial allergens are available. However, fruit and vegetable allergens are very unstable and fresh extracts should be used. Infants can be skin tested for food allergy from 4 months of age.
For this reason, for fruit and vegetable allergens, we tend to use the Prick plus Prick test, where we prick the offending food, gather some sap and then prick the patient with the fresh extract. This form of testing is highly reliable and possibly more accurate than ImmunoCAP RAST tests.
When Skin or Prick plus Prick test are not available, RAST tests should then be used. But many of the RAST fruit allergens extracts are labile and only have a 60% accuracy. They can also be very expensive and blood has to be sent to specialised immunology laboratories to be processed. However, the negative predictive value of food allergy testing is good – if an allergy test is negative, then there is a 90% chance of there being no allergy to that food, but the positive predictive value of allergy testing is less specific – a positive test indicates sensitisation to that food but does not necessarily indicate a clinically relevant allergic reaction is likely occur. This is why we rather discourage allergy screening in otherwise healthy individuals as the results may be misleading.
One should always question whether a specific allergy symptom is linked to a test result, and there is no substitute for years of experience in this field of allergy testing, diagnosis and allergy treatment. The allergy consultation and teasing out of information in the symptom and medical history is pivotal to making the correct allergy diagnosis.
The Double blind placebo controlled food challenge test is the gold standard for food allergy testing and allergy diagnosis, but is totally impractical in the GP setting as it can be very dangerous and trigger anaphylaxis. Only specialised allergy centres with in-house allergy dieticians and full resuscitation equipment are prepared to do this form of allergy testing.
Open food allergy challenge tests (non blinded) using the suspected food allergen are a more practical allergy testing procedure in most allergy clinics as they are less time consuming to perform. Traces of the offending food are given to the person, initially by rubbing allergen onto the skin. Then contact is made with the eyelid or lip. Next traces are placed on the tongue and mouth membranes, until finally an amount of the food is consumed without reaction. Each step of the allergy challenge takes place under close medical supervision at 15-minute intervals. The allergy challenge test is immediately stopped if an adverse reaction is detected at any stage. Experienced medical staff and full resuscitation equipment should always be readily available. Challenge testing should never be done at home without an Epipen readily available.
