Infantile Eczema, also known as Atopic Dermatitis or Atopic Eczema, is a chronic relapsing itchy disease of the skin.
by Dr Adrian Morris
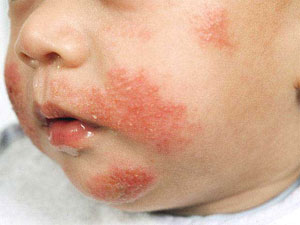 Atopic Dermatitis may commence after the third month of life as a weepy red rash on the face and outer surfaces of arms and legs which itches intensely and then progresses in later childhood into a dry scaly itchy rash commonly of the inner creases of the elbows and knees. There may be associated sandpaper-like roughness of the skin with cracked skin on the palms, around the ears and scaling of the scalp. For this reason, the focus of eczema treatment is to liberally apply copious amounts of moisturisimg ointment-based emollients.
Atopic Dermatitis may commence after the third month of life as a weepy red rash on the face and outer surfaces of arms and legs which itches intensely and then progresses in later childhood into a dry scaly itchy rash commonly of the inner creases of the elbows and knees. There may be associated sandpaper-like roughness of the skin with cracked skin on the palms, around the ears and scaling of the scalp. For this reason, the focus of eczema treatment is to liberally apply copious amounts of moisturisimg ointment-based emollients.
Most often there is a family history of other allergic diseases such as asthma, hay fever and eczema. This family predisposition to allergies is called atopy hence the name Atopic Eczema. Children with atopic eczema tend to have a deficiency of Filaggrin, a protein that binds the skin keratin fibres together and the “barrier” effect of the skin is lost resulting in eczema. Some children may not outgrow eczema and the condition often continues or recurs in adulthood. Adult eczema predominantly affects the neck, ankles and wrists. “It’s not the eruption that itches but the itch that erupts”.
Prevention
Diet
We tend to recommend general allergy prevention measures in high allergy risk newborns. The risk for developing eczema is higher in families who suffer with severe eczema, asthma and nasal allergies. Eczema preventative measures include early application of skin barrier creams such as preservative-free emollients, avoidance of smoking by parents during pregnancy and after birth and breast-feeding until 6 months of age if possible. Some experts suggest avoiding common allergy-provoking foods such as cow’s milk, eggs, fish and peanuts in the breast-feeding mother’s daily diet. However there is no convincing scientific evidence that this really makes any difference. Avoidance of solid foods in babies up to 4 months of age should be followed by the unrestricted phased introduction of the potential allergy-provoking foods such as cow’s milk, wheat, peanut, eggs, sesame and fish slowly one at a time. Recent research seems to indicate that withholding these foods in the first year of life may actually activate food allergies and not be protective as previously thought. Up to a third of infantile eczema is food allergy related and food additives and colourings may also aggravate eczema in older children. Non allergic skin irritation from acidic citrus fruit, tomatoes, pineapples, berry fruits, cheese, chocolate and Marmite, occurs in patients with eczema. Infants may accurately undergo allergy testing for food allergies from 4 months of age.
Clothing
Children should avoid hot humid and cold dry weather, excessive sweating, woollen or synthetic clothing close to the skin and perfumed soaps. Cotton underwear as well as cotton clothing and bed-linen are recommended.
Detergents
Non-biological washing powders should be used instead of enzyme enriched detergents. Add an extra rinse cycle to the wash. Water Softeners attached to the main household water supply help to reduce eczema which is exacerbated by the “hard” British water with it’s high calcium and magnesium salt content. Bubble baths, household antiseptics and perfumed soaps are best avoided. Swimming pool chlorine may also irritate and dry out the skin. Local household skin irritants include wool, mohair, polyester and feathers. Housedust mites, bacteria and dog or cat skin flakes may aggravate eczema.
Bath
Daily bath water should be lukewarm and moisturising emollients must be applied to the skin within 3 minutes of patting the skin dry (never rub the skin dry). If the non-perfumed soaps irritate the skin then rather use aqueous cream, Epaderm or emulsifying ointment as a soap substitute. Add 1/4 cupful of Milton bleach to the bathwater twice a week to clear any skin bacteria that aggravate eczema.
In Bed
As much skin as possible should be covered with non-allergenic lightweight cotton clothing, taking care not to overdress or overheat the child. Cotton night-gloves as well as neatly clipped fingernails will reduce scratching at night whilst asleep. Sometimes elbow splints need to be applied to stop intractable scratching at night. House dust mite exposure may exacerbate eczema and levels of these troublesome mites in the bedroom should be reduced with barrier methods and use of microporous mattress covers.
Immunisations
Routine childhood immunisations and vaccinations should be given. Consult your doctor if you have any concerns about these immunisations. Eczema naturally appears at about age 3 months – unrelated to the first immunisations which are coincidentally given at this time.
Your Career and Eczema
Young adults should decide on a career that is less likely to expose them to irritant chemicals and should probably avoid nursing, hairdressing, catering, motor mechanics, or the building industry. Protective gloves with cotton inner-linings will help prevent irritant contact dermatitis that is so very common in eczema sufferers.
Eczema Treatment
Emollients (use as much and often as possible & ointment better than cream)
These skin moisturising creams and ointments, the mainstay of eczema treatment, are completely safe and should be applied liberally at least three or more times per day to hydrate and protect the skin. Some people may find that a few of these preparations irritate their skin; if this occurs another product should be tried. Different emollients include Emulsifying Ointment (HEB), White Soft Paraffin, 50:50, Aqueous cream (UEA), Doublebase, Diprobase or Lipobase with Cetomacrogol, Epaderm, and Oilatum cream. Choice of emollient is a personal preference, and should be the one that least irritates the skin. Sometimes coal tar is applied to treat thickened skin. Oilatum Plus is an excellent bath emollient. Aveeno is an oatmeal based emollient for very dry skin while Balneum is Soya oil based. As a general rule, all creams are water based and therefore tend to have excipients and preservatives added whereas ointments don’t require preservatives. Arachis Oil derived from peanuts is occasionally used in emollients and may lead to peanut sensitisation.
Steroid Creams (do not be afraid to use to clear eczema)
Steroids produce rapid relief of acute eczema and should be used for short periods of 5 to 7 days to settle eczema flare-ups. They may also be applied for longer periods when diluted 50:50 in an emollient; in which case treatment can be tapered off over a longer period. However, long-term use of concentrated steroids may lead to thinning of the skin. Some of the newer steroid preparations have a much better safety profile. Hydrocortisone 1% is a mild steroid and usually suitable for use on the face to treat eczema, while body eczema usually requires more potent steroid creams such as mometasone, fluticasone and betamethasone and the most potent topical steroid clobetasol should only be used on the hands and feet. Steroid tablets or injections are very rarely, if ever, used in eczema because of their systemic side effects such as stunting growth, eye cataracts and hormonal effects. Topical Steroid Withdrawal Syndrome (TSW) has been highlighted in the media and led to a drop in topical steroid usage. But at normal recommended dosages, topics steroids creams and ointments are unlikely to be problematic.
Wet Wraps (if all else fails)
These are applied at night to keep moisture in the skin, aid absorption of creams and to protected against scratching. First of all, emollients and steroid creams are applied to the eczematous areas. Elasticated cotton-based tubular dressings are soaked in luke-warm water and then cut to size so that they cover the affected areas. These can be applied overnight to the limbs, trunk, neck and even face (holes are cut in the dressing to allow apertures for eyes, ears, nose and mouth). This treatment is highly successful for severe weepy eczema, which is non-responsive to emollients and steroid creams.
Antibiotics (may be needed if eczema fails to clear)
Eczema sufferers are more prone to skin infections such as bacterial, fungal and viral infections, including the common wart and “Ringworm”. Antibiotic creams (Fucidin, Mupirocin) and occasionally oral antibiotics (Flucloxacillin) are prescribed to treat Staphylococcus Aureus infected eczema, which may present as a sudden deterioration of eczema with crusting, oozing and redness of the skin. Staphylococcal colonisation of the skin is a potent trigger for unexplained outbreaks of eczema. Adding a capful of Milton, Dettol or Chlorhexidine 4% gluconate to the bath water may reduce Staphylococcal bacterial colonisation of the skin. Bacterial resistance can occur with prolonged topical use of Fucidin. Hypersensitivity to Malassezia (Pityosporum) yeast on the skin can also lead to worsening eczema and then an anti-fungal shampoo such as Ketoconazole or Selenium sulphide may help eradicate this yeast.
Antihistamines (essential to stop itch and sleep disturbances)
The older sedating type antihistamine tablets or syrup such as Chlorphenamine (Piriton) or Promethazine will reduce itching and subsequent skin damage (excoriation) especially at night. Antihistamine creams may sensitise the skin and should be avoided. Non sedating anti-histamines such as Desloratadine also seem to effectively reduce skin inflammation if used for extended periods of up to 6 months.
Other Therapies (mostly ineffective)
Evening Primrose oil (or gamolenic acid) and Omega 3 oil supplements have proved disappointing in clinical studies on eczema treatment. Extracts of Chinese herbal teas seem to reduce inflammation although they are quite unpalatable and may cause liver damage. Tacrolimus (Protopic) and Pimecrolimus (Elidel) are newer non-steroidal immune modulating creams and results so far have been very encouraging, especially treating eczema on the face, although they may occasionally cause initial reddening and irritate the skin.
Probiotic and prebiotic supplements
In infancy, there is good evidence emerging that colonising the immature bowel with “good” Acidophilus Probiotic microorganisms (Lactobacillus rhamnosus GG and Bifidobacterium) together with Prebiotic supplementation (short-chain oligosaccharides) can delay or prevent atopic eczema developing. These supplements should be taken during pregnancy, breast feeding and in infancy.
Growing clinical evidence suggest that atopic eczema should be treated aggressively in infancy to “train” it and thus reduce recurrences throughout childhood. Modern topical steroid creams are highly effective and are minimally absorbed and at prescribed dosages do not cause adverse effects such as skin thinning.
Reference: Akdis CA, Adkis M, Bieber T et al. Diagnosis and treatment of atopic dermatitis in children and adults: European Academy of Allergology and Clinical Immunology / American Academy of Allergy, Asthma and Immunology / PRACTALL consensus report. J Allergy Clin Imminol 2006; 118: 152-69
