Asthma is a common condition with chronic cough and wheezing, that affects one in five UK children and one in twenty adults.
By Dr. Adrian Morris
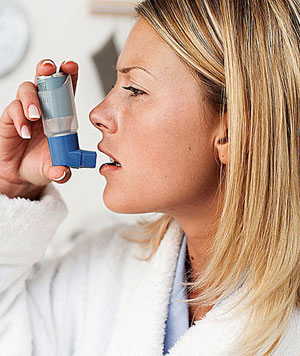 Although asthma usually begins in childhood, and half of those affected will outgrow it by adolescence, it can also occur at any age. There often is an allergic background and a tendency for asthma to run in families, as do related conditions such as eczema and hayfever. Adult onset asthma usually doesn’t have an allergic basis, but may be associated with aspirin sensitivity. Asthma cannot be cured but it can be kept under control so that those affected can live normally and enjoy involvement in sport and other activities. Most asthma sufferers are actually allergic to certain environmental agents such as cats, dogs, house dust mites, pollens and mould spores.
Although asthma usually begins in childhood, and half of those affected will outgrow it by adolescence, it can also occur at any age. There often is an allergic background and a tendency for asthma to run in families, as do related conditions such as eczema and hayfever. Adult onset asthma usually doesn’t have an allergic basis, but may be associated with aspirin sensitivity. Asthma cannot be cured but it can be kept under control so that those affected can live normally and enjoy involvement in sport and other activities. Most asthma sufferers are actually allergic to certain environmental agents such as cats, dogs, house dust mites, pollens and mould spores.
What happens in Asthma?
The typical symptoms of asthma include wheezing, a dry troublesome cough, tightness of the chest and shortness of breath. This is due to narrowing of the air tubes in the lungs – brought on by tightening of the muscles surrounding the airway, inflammation and swelling of the airway lining and production of thick sticky mucous within the airway. This process is usually triggered by a specific allergy or when something irritates the lungs. Daily variation in Peak Expiratory Air-flow of 15% or more confirms the presence of asthma. This diurnal variation is referred to as Peak Expiratory Flow (PEF) Variability. Lowest PEF readings are typically seen in the early morning and highest PEF readings in the evening.
We refer to asthma symptoms that occur occasionally (less than twice a week) and which respond promptly to reliever medication as mild or Intermittent asthma. When asthma becomes more problematic and symptoms occur more often than 2 times per week, with night-time exacerbations; this is then called Persistent asthma and depending on severity would be grade as mild persistent, moderate persistent or severe persistent (where symptoms occur daily and are difficult to control with conventional preventer and reliever treatments).
Asthma triggers
- Asthma attacks are often triggered by allergies to house dust mites, grass and tree pollens, furry pet animals, domestic birds, some foods and mould spores (Cladosporium) at change season.
- A cold or flu can make asthma worse and this effect may persist for up to six weeks unless treatment is adjusted.
- Pollutants in the environment such as cigarette smoke, certain chemicals and car exhaust fumes can trigger an attack.
- Exercise, especially in cold weather, can cause an asthma attack but with correct treatment exercise-induced asthma can be well controlled. Asthmatics should not avoid sport or exercise as in the long-term they are beneficial and increase lung fitness.
- Emotion – anger, anxiety and laughter can all trigger an attack. However, it is not true that “nerves” are the cause of asthma.
- Drinks containing Sulphur Dioxide can trigger asthma attacks.
- Medication such as aspirin, some anti-inflammatory tablets as well as “Beta Blocker” blood pressure tablets and eye-drops for glaucoma may aggravate asthma in adult life.
Asthma Treatment
Asthma cannot be cured but with the right treatment most asthma sufferers can lead completely normal lives. There are two types of treatment: PREVENTER and RELIEVER medication. These are usually given in an atomised form via inhaler devices. We strongly recommend the additional use of a plastic SPACER to increase penetration of the medication deep into the lungs.
It is important to undergo allergy tests to identify which environmental allergens trigger the asthma. This is done by Skin Prick Tests or RAST tests on a blood sample, testing for specific antibodies (IgE) to housedust mites, cats, dogs, pollens, mould spores and cockroaches. Once the specific allergy is identified, avoidance of the allergen may help control symptoms.
Asthma Preventers
These medicines guard against asthma attacks by preventing inflammation and swelling of the mucous membrane lining in the airway of the lungs. They do not give instant relief but their effect is built up over a period of time and they must be used every day continuously.
The original 1970’s asthma preventer medicines such as Sodium Chromoglycate (Intal) and Nedocromil Sodium (Tilade) are no longer available these days. They have been shown to be less effective than low dose inhaled cortico-steroids such as Beclomethasone (Becotide, Clenil, Qvar, Asmabec), Fluticasone (Flixotide), Budesonide (Pulmicort), Mometasone (Asmanex) and Ciclesonide (Alvesco) which are the mainstay of asthma prevention and control . All of these medicines are very safe to use at the recommended dosages and SHOULD BE USED CONTINUOUSLY EVEN WHEN SYMPTOM FREE.
Newer oral preparations called Leukotriene Antagonists are available and include Montelukast (Singulair) and Zafirlukast (Accolate). Monoclonal anti-IgE antibodies in the form of Omalizumab (Xolair) have a profound effect on severe allergic asthma which is difficult to control, this treatment involves injections every 4 weeks and is expensive but life saving in brittle asthma.
Asthma Relievers
These medicines will help patients with breathing difficulties during an asthma attack. They relax the muscles surrounding the bronchial tubes and give instant relief of symptoms. If they need to be used frequently, it is an indication that the asthma is poorly controlled and the dosage of Preventer treatment should be increased. If the dose used increases to more than the doctor has recommended, please contact your doctor about this. Reliever medicines include Salbutamol (Ventolin, Airomir, Asmasal), Terbutaline (Bricanyl), Bambuterol (Bambec), Fenoterol (Berotec) and Ipratropium (Combivent & Duovent).
Longer acting bronchodilator (LABA’s) relievers are also called Controllers and Salmeterol (Serevent) plus Formoterol (Oxis, Foradil) are popular examples which are used twice daily, but usually recommended as add-on treatment to inhaled steroids. Current recommendations are that LABA’s should always be used in conjunction with inhaled steroids which reduce airways inflammation.
As better treatments have evolved, older oral preparations such as the Theophyllines and Aminophylline are rarely prescribed these days.
Combination Preventer and Long-Acting Beta Agonist (LABA) reliever inhaler medications are Seretide and Symbicort. Seretide, which is a combination of Salmeterol and Fluticasone have a synergistic or additive effect in asthma control and treatment. Symbicort is another new combination preventer and controller inhaler which contains Budesonide and Formoterol. A new longer-acting reliever inhaler (LABA) called Vilanterol may have a 24 hour duration of action.
There is no direct connection between the effects of reliever and preventer medicines. They have quite separate actions on the lung airways.
Bronchial Thermoplasty is a new treatment in severe asthma whereby the thickened airway bronchial muscle (which makes the asthma difficult to control) is destroyed by heat using a bronchoscope (lung probe) to relieve airway spasm. It usually involves a series of treatments.
Complementary treatments are often incorrectly called “alternative” treatments; there are no effective alternatives to modern medication in asthma treatment. Homeopathy, herbal Butterbur, Buteyko and breathing exercises are not as good as conventional treatment. If you decide to consult someone other than your doctor, remember to continue using your preventer and reliever medicines.
Asthma Treatment
It is very important to recognise when asthma is getting worse.
Asthma that gets worse at night or in the early hours of the morning indicates a need for additional treatment. Wheezing or a tight chest that is not relieved by several reliever inhalations, particularly if there is difficulty with talking, necessitates urgent medical assistance.
Those asthmatics that are often troubled with asthma attacks should have their own PEAK FLOW METER at home so that they can measure their lung performance and know when extra treatment or medical advice is necessary. Discuss an Asthma Management Plan with your doctor – you may need a short course of oral Steroid tablets at home to take in an emergency.
Your doctor or Practice Nurse will develop a STEPWISE ASTHMA MANAGEMENT PLAN with you which will explain how to use the preventer and reliever medication and what to do if the asthma gets worse.
The most common cause for poor asthma control is not using adeqaute Preventer (low dose steroid) inhalers and relying too much on Reliever (bronchodilator salbutamol) inhalers.
Chronic cough and types of asthma
Various different types of asthma have been identified over the years.
Classical asthma: Typically reversible wheezing and airways bronchospasm, associated with eosinophils in the mucous and which responds well to bronchodilators (salbutamol) and inhaled steroids (beclomethasone).
Cough-variant asthma: (first described in 1972) This dry cough responds well to broncho-dilators (implying presence of bronchospasm) and is associated with a very sensitive cough-reflex. This is a common condition in small children and one third will progress to develop Classical asthma.
Eosinophilic bronchitis: An isolated chronic cough seen in adults and associated with eosinophils in sputum, but no airways bronchospasm or wheeze. This condition may progress to fixed airway disease such as occurs in chronic bronchitis and emphysema. This cough does not respond to broncho-dilators but does improve with inhaled steroids.
Atopic cough: (a recently identified asthma variant). This isolated chronic cough in children is not associated with airways bronchospasm or wheeze. There is usually a family history of allergy, and allergy skin tests are positive with raised IgE, however there are no eosinophils in the sputum. This cough responds well to antihistamines (cetirizine, loratidine or chlorpheniramine) and inhaled steroids but not at all to bronchodilators (salbutamol). It does not usually progress to Classical asthma.
Certain conditions such as Acute Bronchopulmonary Aspergillosis (a fungal infection and allergy in the air tubes) and Extrinsic Allergic Alveolitis (Farmer’s Lung) should be considered if people with asthma-like symptoms do not respond to standard asthma therapies. Occupational asthma may occur in Bakers and also with chronic exposure to isocyanates, wood dust, platinum salts and animal allergens (in veterinary workers)
The National Asthma Campaign has practical booklets on asthma treatment and also will let you have an “asthma diary” to log Peak Flow measurements and symptoms. We also recommend a visit NHS Choices for more information https://www.nhs.uk/conditions/asthma/
Wikipedia also has more information on asthma testing.
If you or a family member are experiencing symptoms of asthma such as wheezing, tight chest, shortness of breath and coughing, please contact Dr. Morris.
