Urticaria is a raised, itchy and painful rash that migrates about on the skin. It is also called a “nettle rash” or hives. Angioedema swelling is when the deeper tissues are affected with swelling and pressure on airways (previously called Angioneurotic Oedema). Urticaria is common affecting 15 to 30% of the population some time in their life.
by Dr Adrian Morris
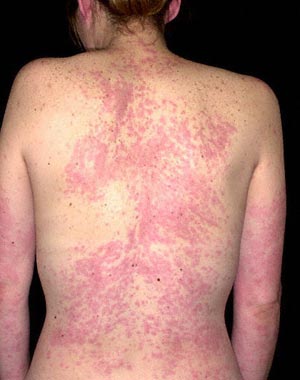
Introduction
There are distinct types of urticaria called Spontaneous Urticaria and Inducible Urticaria (also known as Physical Urticaria). Ordinarily spontaneous urticaria has two patterns – Acute Urticaria and Chronic Urticaria.
- Acute urticaria is most often caused by an allergy to food, insect sting, viral illness or medication and can last between several hours and six weeks.
- Chronic urticaria is diagnosed if the rash persists or recurs for six weeks or longer, the underlying cause is then usually not due to food allergies
All forms of urticaria may occur in association with deeper skin swelling or angioedema and equally, angioedema may occur in isolation with no apparent urticaria. This depends on whether we release histamine into the skin (urticaria), deeper tissues (angioedema) or both. Angioedema swelling is most apparent in lax tissues around the eyelids, lips, tongue and genitals. This is also referred to as Angioneurotic oedema and can be associated with Anaphylactic shock.
Just to confuse the issue, Chronic Urticaria may also occur together with Physical (Inducible) Urticaria.
Urticaria causes
Acute Urticaria
The most likely cause of Acute Urticaria is an allergy due to exposure to pets, horses, latex rubber, food such as shellfish, nuts, egg and dairy products or bee and wasp stings. Allergies to medication such as antibiotics (penicillin, tetracycline, sulphonamides and cephalosporins), blood pressure pills (ACE inhibitors and diuretics), codeine and aspirin containing pain killers can cause acute urticaria.
The most common cause for Acute Urticaria in a child will be a viral infection (Viral Urticaria). Sometimes viral infections such as glandular fever and hepatitis B, or bacteria (helicobacter, mycoplasma, streptococci), fungal and parasitic infections can trigger urticaria in adults. Allergic reactions to blood products, transfusions, xray contrast and vaccines have also been implicated. Papular urticaria is the medical term for “itchy bumps” or grouped urticarial lesions seen mainly in children and which follow insect bites from midges, fleas and mosquitoes. Skeeter Syndrome is an localised allergic skin reaction to proteins from a mosquito bite.
Chronic Urticaria
The cause of Chronic Urticaria is much more difficult to identify it may be inducible or spontaneous. The role of true food allergy is hardly ever a significant trigger but food additives such as salicylate, sodium benzoate, sulphites, artificial colourings and nitrites may play a role. We often end up diagnosing Chronic Spontaneous Urticaria (previously called Chronic Idiopathic Urticaria) when no cause is identified. This condition (which can persist for many years) is due to the production of “auto-antibodies” which in turn attack specific Mast Cells in our skin and tissues causing an enormous release of histamine. Activation of the coagulation cascade may also be implicated.
Why we suddenly switch-on production of these aggressive antibodies to our own skin cells is a complete enigma. Our bodies may continue producing these auto-antibodies for a number of years leading to a great deal of distress and discomfort for the urticaria sufferer. Unfortunately over 50% of Chronic Urticaria cases are due to production of these “auto-antibodies” to the IgE and its receptor on Mast Cells found in the skin; hence there is a possible relationship to underlying thyroid and joint diseases. 30% of cases of Chronic Urticaria have underlying silent thyroid disease (Hashimoto’s Thyroiditis). Female to male preponderance is 5:1.
Chronic undetected dental, sinus, urinary or parasitic infections as well as ACE inhibitor blood pressure pills (lisinopril, ramipril, enalapril and perindopril) may play a role in triggering chronic urticaria. Stress is known to aggravate urticaria and stress reduction measures are very important in treating chronic idiopathic urticaria. A scoring system for urticaria (measuring wheals & itch) using a 7 day activity score – Urticaria Activity Score (UAS7) has been devised to monitor activity and response to treatment.
Physical Urticaria
Physical urticaria or Inducible Urticaria can be triggered by physical factors such as exposure to environmental heat (prickly heat), intense cold (cold urticaria), sunlight (solar urticaria), water (aquagenic urticaria), vibration from pneumatic drills or pressure on the skin from tight clothing. Lesions typically last less than one hour. Exercise and sweating may trigger a fine itchy rash called Cholinergic Urticaria. Very rarely some people are allergic to all forms of water, this is called “Aquagenic” Urticaria. Exercising shortly after eating certain foods such as wheat, celery and shellfish might provoke delayed urticaria, asthma or even anaphylaxis.
Many people have very sensitive skin and any friction or rubbing will cause raised red lines to develop (FricTest). This is called Dermatographism or Dermographia and indicates just how easily they can release histamine into their own skin. A good test for Cold Urticaria is to hold a block of ice against the skin for 5 minutes and see if an urticaria weal develops after the ice is removed. Whereas pressing a blunt pencil against the skin for one minute will lead to a wheal developing immediately in Pressure Urticaria, while in Delayed Pressure Urticaria the wheal may only develop after 6 hours.
Underlying thyroid diseases and autoimmune diseases such as Thyroiditis, Systemic Lupus and Rheumatoid Arthritis can provoke Chronic Urticaria or even Urticarial Vasculitis (a variant in which the lesions tend not to fluctuate but lead to skin bruising). Urticarial Vasculitis may be associated with a fever, bone pains and joint swelling (Schnitzler’s Syndrome). Henoch Schonlein purpura is a common “urticarial” vasculitis occuring on the lower limbs in children and occasionally children with Coeliac Disease may present with urticaria. Very often Chronic Idiopathic Urticaria will be accompanied by Physical Urticaria.
Contact Urticaria results in immediate localised skin lesions on the hands or exposed skin from direct skin contact with urticaria triggers such as latex, cosmetics, perfume and food preparation (seafood & potato)
Occasionally an inherited deficiency of the C1 Esterase Inhibitor Enzyme leads to a non-itchy form of urticaria called Hereditary or Familial Angioedema. This condition affects mainly females in a family, is associated with sudden swelling of the face and neck which is painful, but there is no rash. These lesions usually last for 2 to 3 days and do not respond well to antihistamine medication. Sufferers characteristically have low levels of the Complement C4 (<0.12g/l) in their bloodstream and respond to medication such as Danazol or Tranexamic acid which prevent angioedema attacks. Isolated angio-oedema without urticaria may also be triggered by aspirin, ibuprofen, epilepsy and blood pressure medications.
Urticaria symptoms
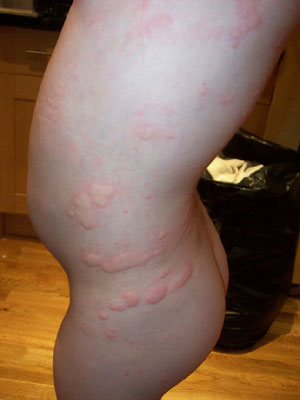 Lesions tend to move about every 24 hours and “migrate” around on the body.
Lesions tend to move about every 24 hours and “migrate” around on the body.
In chronic cases, the intense itchiness will cause sleepless nights and may lead to a depressive illness. Chronic urticaria tends to fluctuate by temporarily settling down and then suddenly relapsing again with co-existent viral illnesses, stress and aspirin containing medication such as flu remedies. This chronic pattern may recur for 5 years to 20 years in some cases!
If your urticaria does not disappear after a few weeks, or does not respond to antihistamine medication, and is accompanied by any other health problem, you should go to your doctor. Blood tests may help identify an allergy or underlying immune disorder but most often all tests come back normal. A rare but troublesome cause for chronic urticaria is Systemic mastocytosis where there is a total over abundance of Mast Cells in the body with raised levels of Tryptase in the bloodstream. Localised Mast Cell overproduction in the skin is associated with excessive pigmented freckles and called Urticaria pigmentosa (then the urticaria is elicited by firmly rubbing the skin – called Darier’s sign).
Urticaria treatment
Avoid any obvious triggers or exacerbating factors and try these simple measures:
Keep the skin cool, avoid getting hot from exercise and take lukewarm baths. Resist the temptation to rub the itchy skin and apply copious amounts of moisturising creams to reduce dryness and itch. Avoid alcoholic drinks, anti-inflammatory drugs and foods containing additives and pseudoallergens (sodium benzoate, sulphite preservatives, colourings and salicylate).
- Apply 1% menthol in aqueous cream or Eurax to soothe the affected skin
- Avoid all aspirin or codeine containing medication (including ibuprofen, diclofenac, indomethacin, naproxen and mefenamic acid). Only use simple paracetamol as a painkiller
- Avoid ACE inhibitor blood pressure pills (lisinopril, ramipril, enalapril & perindopril), if you are prone to developing urticaria and angioedema
- Carefully read Side Effects list of any other medication you are currently taking and avoid medicines that are known to trigger urticaria or angioedema
- Pregnancy may specifically aggravate urticaria as Pruritic and Urticarial Papules and Plaques of Pregnancy (PUPPP syndrome)
- Stress, overheating, tight clothing and alcohol may aggravate and make urticaria worse.
- A diet containing low-histamine containing foods (avoiding dark fish, spinach, avocado, berries, banana and strong cheeses) and other pseudo-allergens and preservatives (adapted Berlin Diet) may be helpful by reducing the “histamine load” on chronic urticaria. Green Tea may provoke urticaria and should be avoided.
The mainstay of urticaria treatment is high dose (second generation) antihistamine medication which may be necessary for prolonged periods (in excess of 6 weeks). Up to quadruple the conventional doses of these non-sedating antihistamines such as Cetirizine, Loratadine, Acrivastine and Fexofenadine may be needed to get symptom relief. The new “isomers” called desloratadine and levocetirizine don’t seen to offer any additional benefit in treating urticaria. Long-term deal steroids such as Prednisolone should be avoided due to adverse side effects.
Traditionally we add “stomach-ulcer treatment” medication such as Cimetidine and Ranitidine which are known to also dampen down histamine release. Ranitidine containing a chemical NDMA has been implicated in a recent cancer scare. Occasionally we need to add sedating antihistamines such as Chlorphenamine or Hydroxyzine at night to get urticaria control. Leukotriene receptor antagonists currently used for asthma such as Montelukast (leukotriene receptor antagonists) have provided some symptom relief in a few cases of chronic urticaria when used in combination with antihistamines. Oral antidepressant Doxepin is a good antihistamine but may induced drowsiness, while Doxepin cream (if available) can soothe the skin.
Short courses of oral cortisone or steroids may be necessary for short periods (up to 5 days) to settle more severe symptoms and get control, however rebound urticaria after steroid use is a problem. Cortisone (Prednisolone) should not be used for prolonged periods of time as this may lead to stunted growth in children and osteoporosis in adults, therefore Kenalog (long acting)) steroid injections are discouraged. Although steroids initially suppress chronic urticaria, we find that on stopping them, the urticaria tends to rebound and become more diffficult to treat. Chlorphenamine and Loratadine are safe to use in early pregnancy, while Cetirizine and Loratadine are safe to take whilst breastfeeding.
Specialist urticaria testing
Historically chronic urticaria was thought to be due to stress and food allergies, but this is actually not the case. 80% of cases are idiopathic (we find no cause) due to auto-antibodies and coagulation cascade activation. Specialist urticaria testing in Chronic Urticaria may be necessary to exclude other underlying illnesses or to confirm the presence of “auto-antibodies” in the blood stream (“Anti IgE Receptor Autoantibodies” and “Basophil Histamine Release” can be measured). The Autologous Serum Skin Test (ASST) raises a weal on re-injection of the patients serum and is a good indicator of Auto-antibodies. In more severe persistent urticaria, a skin biopsy of a lesion shows a preponderance of Eosinophils over Neutrophils and the patient will often have a raised D-dimer test indication coagulation cascade activation as a trigger for the urticaria.
Highly specialised third line treatments may include Immunosuppressive drugs such as Ciclosporin (autoimmune urticaria), Methotrexate (non-autoimmune urticaria), and Sulphasalazine (Pressure urticaria). Androgen hormones, Thyroxine, Nifedipine and Warfarin have been used with variable efficacy as well. Colchicine and Dapsone are useful in treating Urticarial Vasculitis. If available, Immunoglobulin injections, Plasmaphoresis have been used. The use of a an asthma drug, the anti-IgE monoclonal antibody Omalizumab (Xolair) may be necessary if no other treatment is effective. Although expensive at £ 500 per month, the drug is very effective at clearing chronic urticaria and has been approved as second line therapy for Chronic Urticaria by the US (FDA) and UK (NICE) guidelines. However when the treatment is stopped , the urticaria tends to recur.
Reference:
Powell RJ, Leech S, Till S et al, BSACI guidelines for the management of chronic urticaria and angio-oedema. Clin Exp Allergy 2015: 45; 547-565.
Greaves MW, Kaplan AP. Urticaria and Angioedema (Marcel Dekker 2004)
The British Association of Dermatologists supply useful information of the public.
NHS Choices website also supplies additional information on controlling urticaria.
