The most commonly used diagnostic test in food allergy is Skin Scratch Testing (SPT) with extracts of fresh food allergens or specific IgE testing (RAST test) on a blood sample.
by Dr Adrian Morris
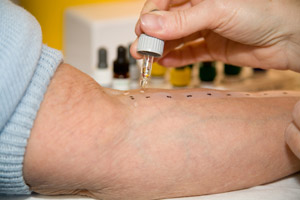 Skin Scratch Allergy Testing is the cornerstone in allergy diagnosis, it has been used for over 100 years. Skin allergy testing is cheap, safe, easy to do and someone in the practice can easily be trained to perform it. Commercial inhalant allergens are readily available, but food allergens are a little more difficult to come by. The main problem with food allergens is the lack of stability of extracts. A few food allergens such as Peanut, Hen’s Egg, Wheat, Soy bean, Tree nuts, Fish and Cocoa are stable and commercial allergens are available. However, fruit and vegetable allergens are very unstable and rapidly denature rendering commercial extracts less reliable. Infants can be allergy tested on the skin for food allergy from 4 months of age.
Skin Scratch Allergy Testing is the cornerstone in allergy diagnosis, it has been used for over 100 years. Skin allergy testing is cheap, safe, easy to do and someone in the practice can easily be trained to perform it. Commercial inhalant allergens are readily available, but food allergens are a little more difficult to come by. The main problem with food allergens is the lack of stability of extracts. A few food allergens such as Peanut, Hen’s Egg, Wheat, Soy bean, Tree nuts, Fish and Cocoa are stable and commercial allergens are available. However, fruit and vegetable allergens are very unstable and rapidly denature rendering commercial extracts less reliable. Infants can be allergy tested on the skin for food allergy from 4 months of age.
For this reason, for fruit and vegetable allergens, we tend to use the Prick plus Prick test, where we prick the offending food, gather some sap and then scratch the patient with the fresh extract. This form of allergy testing is highly reliable, reproducible and possibly more accurate than RAST allergy tests. We often ask patients to bring some fresh samples of suspected food allergens along to the clinic appointment so that we can prepare an allergy test reagent directly to suspected food allergens at the initial consultation.
Alternatives to Skin Scratch Allergy Testing
If Skin allergy testing is not available, RAST IgE tests are an accurate alternative. Occasionally false positive test results may occur and RAST tests have a 80% accuracy. They can be expensive if many allergens are tested and blood has to be sent to specialised immunology laboratories to be processed. Screening tests such as ISAC and ALEX are much more cost effective. The negative predictive value of food allergy testing is good – if an allergy test is negative, then there is a 90% chance of there being no allergy to that food., but the positive predictive value is less specific – a positive test indicates sensitisation to that food but does not necessarily confirm a clinical allergic reaction will occur when next exposed.
Atopy Patch Tests on the skin detect delayed hypersensitivity allergic reactions, usually to contact allergens such as nickel, rubber and cosmetics. However a new application of this patch test is to allergy test for food allergens especially where a delayed hypersensitivity reaction is suspected in children as in infantile eczema. The food allergen is applied to the skin under an occlusive cover (called a Finn chamber) and the skin is assessed after 48 and 72 hours for a wheal reaction. Testing for preservative allergy can also be undertaken with Patch Testing for delayed hypersensitivity to Sulphur Dioxide (Sulphites) and Sodium Benzoate found in foods and condiments such as wine, dried processed fruits, Balsamic vinegar, tomato sauce and relish.
The skin test and RAST allergy tests are the conventional allergy tests that have been subjected to the most rigorous research and have been shown to be reliable, reproducible and accurately detect allergic reactions to foodstuffs.
The Double blind placebo controlled food challenge test is the gold standard for food allergy diagnosis, but is totally impractical in the GP setting as it can be very dangerous and trigger anaphylaxis. Only specialised allergy centres with in-house allergy dieticians and full resuscitation equipment are prepared to do this form of allergy testing. Open food challenges (non-blinded) with the suspected food allergen is the more popular procedure in most clinics. Traces of the offending food are introduced to the person, initially by rubbing onto the skin. Then contact is made with the eye or lip. Next traces are placed on the oral mucous membranes, until finally a substantial amount of the food is consumed without allergic reaction. These allergy challenges take place under close medical supervision at 15-minute intervals. The test is stopped if an adverse reaction occurs at any stage.
Conventional IgE Blood Allergy Testing
(RASTs and ImmunoCAP)
The newer RAST allergy tests are called ImmunoCAP RAST allergy tests and measure specific IgE in the serum to different food allergens. To simplify matters, there are various screening panels.
In children the common food allergens are contained in the fx5 Paediatric Food Allergy Screen, and these are Cow’s milk, Hen’s egg white, Wheat, Soya, Peanut and Codfish. There is a Nut Screen called fx1, which contains Brazil nut, Hazelnut, Almond, Coconut and Peanut. Then there is a Seafood mix called fx2 that contains Codfish, Shrimp, Blue mussel, Tuna, and Salmon. The Cereal mix screen called fx3 contains Wheat, Oat, Maize, Sesame seed and Buckwheat. Another useful food allergy screen is the fx7, which mix contains Tomato, Yeast, Garlic, Onion and Celery.
There are up to 160 different food allergens that can be used to allergy test for specific IgE antibodies, and range from Almond through to Youngberry.
Some foods such as cow’ milk and certain fruits contain a large number of different potential allergens and one has to be aware that a specific RAST may only allergy test a few of the potential allergens in the food thereby missing minor allergens. Some people who are perhaps sensitised to a minor allergen in a particular food may RAST allergy test negative, when in fact they are allergic to that food. New component allergen testing is available for specific component allergens found in a food which can identify anaphylaxis risk in foods such as peanut Ara h 2 and peach Pru p 3, just to mention two important component allergens.
Pitfalls in food allergy diagnosis
Food Cross-reactions occur within so called botanical food families. If you are allergic to one food, then you may develop allergies to other foods within the same food family. For instance, Peanut is a member of the legume family and so peanut allergic people may cross react with soya, peas, chickpeas, lentils, beans, senna, liquorice or carob (these cross-reactions are surprisingly uncommon).
More commonly allergic reactions occur to widely distributed allergens called Panallergens (Lipid Transfer proteins and Profilins) – one is the allergen in Silver Birch Pollen, this often cross reacts with other profilins in foods from diverse botanical families such as apple, hazelnut, cherry and celery. As a consequence, people suspect they are allergic to only one fruit but end up having reactions to a number of unrelated fruits and vegatables. This is diagnosed using the ISAC component allergen screening blood test which measures IgE antibodies to over 100 component allergens.
Cooking tends to denature food allergens, so people will tolerate the food if cooked or canned. This commonly occurs with fruit and vegetables. But if the allergen happens to be heat stable such as with peanut and fish – cooking does not denature or reduce the allergenicity. In the case of peanuts, roasting at high temperatures actually increases the allergy potential
As fruit or vegetables ripen, they become more allergenic – hence green tomatoes may be tolerated, but fully ripened ones cause a severe allergic reaction in a tomato sensitive person.
Clusters of Hypersensitivity
(Foods that have cross-reacting allergy with one another)
Similar pan-allergens or profilins occurring naturally in different fruit families, lead to what we call “clusters of hypersensitivity”. For example if you are allergic to Brazil nut, you stand a high chance of also being allergic to walnut and pecan nut. And similar patterns are seen with Onion, Leak and Garlic; Bean, Pea, Chickpea and Lentil; Parsley, Carrot and Celery; Cashew, Mango and Pistachio. Even between Pumpkin, Melon, Watermelon, Courgette and Cucumber!
Sensitisation to PR-10 pan-allergen and other Lipid Transfer Proteins (LTP) lead to further fruit sensitisation as new fruits enter the diet. This usually occurs in pollen allergic people who suffer with seasonal rhinitis or hayfever.
Drawbacks of Conventional Allergy Tests
There are a few drawbacks to food allergy testing which make it a less-than-exact science.
At present we can only reliably measure IgE antibodies and diagnose IgE mediated food allergy with any accuracy. However we suspect other mechanisms may be implicated such as Delayed T-cell mediated hypersensitivity allergic reactions and direct Basophil Histamine release. In these cases, it would be more useful to measure cellular leukotriene release. These leukotriene inflammatory mediators are released directly in many medication and food additive allergic reactions and dont involve IgE at all. But commercially available allergy tests for these reactions such as CAST (Cellular Allergen Stimulation Test) testing is difficult to interpret with a reasonably good positive predictive value but poor negative predictive value. So in the meantime due to a lack of accurate tests, we do not actually know the extent of these non-IgE allergic reactions.
Another large area in adverse food reactions are those allergic reactions to Food Additives that we know are not IgE mediated. Only challenge testing can confirm food additive intolerance and this can be most unpleasant and even dangerous for some patients. At present, we have to eliminate the food, and note a clinical improvement, then re-challenge the patient to confirm the adverse allergic reaction.
Provocation allergy testing whether open or double blinded is to dangerous in General Practice and non-acute hospitals and should only be done in specialist allergy centres. They are very time consuming and tedious to perform and often manpower is not available to make this a viable allergy diagnostic option.
Delayed allergic reactions and intolerances to foods are much more difficult to confirm on testing as they very often do not involve the IgE antibody immune system. Often the mechanism behind the delayed allergy may differ and time scale from exposure to reaction may vary. Immunoglobulin G (IgG) testing to identify type III delayed allergic reactions have been explored and IgG antibody test technology has been improved. However, to date there have been no convincing clinical studies that have concluded that IgG testing is an accurate method of confirming the cause of delayed food reactions or food intolerance/sensitivity. Despite these findings, some commercial organisations still routinely advertise on the internet and perform IgG antibody tests to “confirm” the presence of food intolerance and recommend temporary diet changs.
Lactose intolerance cannot be diagnosed on a blood or skin allergy test. It is reliably diagnosed with a “hydrogen breath” test or reducing sugars (acids) measured in the diarrhoeal stool after 250ml low fat milk. For gluten intolerance or gliaden sensitivity such as occurs in Coeliac disease which affects 1:100 people, see our section “Coeliac Disease” in the contents bar. For reliable testing the diet needs to contain gluten for at least 4 to 6 weeks.
For further information on allergy testing we recommend a visit to the NHS Choices website https://www.nhs.uk/conditions/allergies/diagnosis/
The UK charity Allergy UK also provides additional information https://www.allergyuk.org/information-and-advice/conditions-and-symptoms/585-managing-my-food-allergy
View a video of allergy skin testing >
